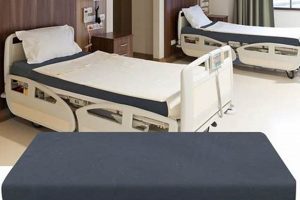
A specialized support surface is designed for use in adaptable hospital beds that can transition between acute and skilled nursing care settings. This type of bedding provides comfort and pressure redistribution for patients who may require extended periods in bed due to illness, injury, or post-surgical recovery. For example, a patient recovering from a hip replacement might utilize this bedding during their initial hospital stay and subsequent rehabilitation within the same facility.
The implementation of appropriate support surfaces offers numerous advantages. These include enhanced patient comfort, reduced risk of pressure ulcer development, and potentially shortened rehabilitation periods. Historically, the provision of such bedding has been a key component in providing comprehensive care, enabling healthcare facilities to optimize resource allocation and improve patient outcomes. Its use allows facilities to offer a continuum of care without unnecessary patient transfers.
The following sections will delve into the specific characteristics, construction materials, and selection criteria for optimal bedding choices in this specialized care setting. Further discussion will cover the regulatory aspects and best practices for maintaining hygiene and extending the lifespan of these essential medical devices.
Essential Considerations
This section offers crucial guidance for effectively utilizing and maintaining specialized bedding within a swing bed setting. Adhering to these points promotes optimal patient care and extends the lifespan of the equipment.
Tip 1: Pressure Redistribution Assessment: Regularly evaluate the patient’s skin integrity and risk factors for pressure ulcer development. Implement a documented schedule for repositioning patients, considering individual needs and the specifications of the particular support surface. For example, high-risk patients might require repositioning every two hours.
Tip 2: Compatibility Verification: Ensure the selected support surface is fully compatible with the swing bed frame’s dimensions and adjustable features. Incompatible bedding may compromise the bed’s functionality and potentially create safety hazards for both patients and caregivers.
Tip 3: Infection Control Protocols: Strictly adhere to established infection control protocols when handling and cleaning the bedding. Utilize appropriate cleaning agents and disinfection techniques as recommended by the manufacturer. This minimizes the risk of cross-contamination and healthcare-associated infections.
Tip 4: Proper Storage Practices: When not in use, store the bedding in a clean, dry environment, protected from direct sunlight and extreme temperatures. Incorrect storage can lead to material degradation and reduced performance.
Tip 5: Weight Capacity Adherence: Always verify and strictly adhere to the weight capacity specified by the manufacturer. Exceeding the weight limit can damage the bedding and compromise its ability to provide adequate support and pressure redistribution.
Tip 6: Regular Inspection and Maintenance: Conduct routine inspections for signs of wear, damage, or deterioration. Promptly address any identified issues, such as tears, punctures, or compromised seams, to maintain optimal performance and prevent further damage.
Effective utilization and maintenance of specialized bedding are paramount for delivering quality care in a swing bed setting. Compliance with these guidelines will contribute to enhanced patient comfort, reduced risk of complications, and extended equipment longevity.
The subsequent sections will provide additional insights into specific types of bedding materials and advanced technologies employed in modern support surfaces.
1. Pressure Redistribution
Pressure redistribution is a critical characteristic influencing the effectiveness of hospital bedding, especially within swing bed settings. The primary function of specialized support surfaces is to minimize concentrated pressure on bony prominences, thereby preventing or mitigating the development of pressure ulcers. This is achieved through materials and designs that conform to the patient’s body, distributing weight across a broader surface area. Failure to effectively redistribute pressure can lead to localized ischemia, tissue damage, and the formation of debilitating ulcers, particularly in patients with limited mobility or compromised circulatory systems.
The effectiveness of pressure redistribution is directly correlated to the materials used in construction. Viscoelastic foam, air-filled bladders, and gel-infused layers are common components designed to contour to the patient’s body and relieve pressure points. For example, a hospital employing bedding with advanced air-redistribution technology may observe a significant reduction in the incidence of Stage II or higher pressure ulcers compared to facilities using standard innerspring mattresses. The choice of material and the engineering of its distribution are, therefore, integral to patient outcomes and cost savings associated with reduced wound care.
In summary, pressure redistribution is not merely a feature of specialized hospital bedding; it is a fundamental requirement for preventing patient harm. Understanding the principles of pressure redistribution, the materials that facilitate it, and the potential consequences of inadequate implementation is essential for healthcare providers aiming to optimize patient care and minimize healthcare-associated complications. Selecting appropriate bedding based on a patient’s risk factors and clinical needs, coupled with vigilant monitoring of skin integrity, is paramount for achieving positive clinical outcomes.
2. Material Composition
Material composition is a defining factor in the performance and suitability of hospital bedding, impacting everything from patient comfort to infection control. The specific materials used directly influence pressure redistribution capabilities, durability, and the ability to withstand rigorous cleaning protocols essential in healthcare environments. For instance, a surface constructed with high-density memory foam will offer superior contouring and pressure relief compared to a standard innerspring mattress, reducing the risk of pressure ulcer development in patients with limited mobility.
The choice of materials also affects infection control. Surfaces constructed with impermeable, antimicrobial-treated fabrics prevent the absorption of fluids and the proliferation of bacteria. Polyurethane-coated nylon, for example, provides a durable, wipeable surface that can withstand frequent disinfection with hospital-grade cleaning agents. Conversely, bedding with porous or damaged surfaces can harbor pathogens, increasing the risk of healthcare-associated infections. Furthermore, the durability of materials dictates the lifespan and cost-effectiveness. While a less ex
pensive vinyl-covered surface may initially appear attractive, it is often prone to cracking and tearing, necessitating frequent replacement and potentially exposing patients to compromised hygiene.
Ultimately, the selection of materials constitutes a critical decision that impacts patient safety, clinical outcomes, and the financial sustainability of healthcare facilities. A comprehensive understanding of the properties, advantages, and limitations of various materials is paramount for making informed decisions that prioritize patient well-being and operational efficiency. Considering factors such as pressure redistribution, infection control, durability, and patient allergies is crucial in choosing the appropriate bedding for diverse patient populations and clinical settings.
3. Infection Control
Infection control is paramount in healthcare settings, and bedding within a swing bed unit presents a unique set of challenges due to the dual-purpose nature of the beds. These beds accommodate both acute and sub-acute care patients, potentially exposing them to a wider range of pathogens. Inadequate infection control practices related to bedding can directly contribute to healthcare-associated infections (HAIs), increasing morbidity, mortality, and healthcare costs. For example, porous or damaged mattresses can harbor bacteria, viruses, and fungi, even after standard cleaning procedures. A single contaminated bed can become a reservoir for pathogens, leading to outbreaks within the facility. The materials used in the construction of the bedding must be carefully selected to facilitate effective disinfection and prevent microbial growth.
Further, consider the impact of surface integrity. Tears, cracks, or compromised seams in the protective covering can provide entry points for bodily fluids, creating an environment conducive to microbial proliferation. Regular inspection and prompt repair or replacement of damaged bedding are essential. The cleaning protocols must be rigorous and consistently followed, utilizing appropriate disinfectants with proven efficacy against common healthcare-associated pathogens. Staff training on proper handling and cleaning procedures is crucial for maintaining a safe environment. Some facilities have adopted disposable barrier technologies, adding an extra layer of protection between the patient and the mattress surface. Such measures minimize the risk of cross-contamination and enhance overall infection control efforts. The implementation of ultraviolet (UV) disinfection technologies to sanitize bedding surfaces represents another proactive approach to reduce pathogen loads.
In conclusion, effective infection control strategies pertaining to specialized bedding are indispensable for patient safety and quality of care. The interplay between material selection, surface integrity, cleaning protocols, and staff training determines the effectiveness of these strategies. Recognizing the inherent risks associated with compromised bedding and implementing proactive measures to mitigate these risks are essential components of a comprehensive infection control program. Prioritizing infection control in the selection and maintenance of specialized bedding is not merely a matter of compliance but a moral imperative for healthcare providers.
4. Weight Capacity
Weight capacity is a critical parameter directly impacting the safety and efficacy of specialized bedding within a swing bed setting. Exceeding the designated weight limit compromises the intended functionality of the support surface and presents potential hazards for both the patient and the equipment.
- Structural Integrity and Support
The stated weight capacity ensures the structural integrity of the bedding. Exceeding this limit can lead to deformation, compression, or even complete failure of the internal support components, such as foam layers, air bladders, or coil systems. Compromised structural integrity reduces the effectiveness of pressure redistribution, increasing the risk of pressure ulcer development. For instance, a surface rated for 300 lbs may not provide adequate support or pressure relief for a patient weighing 350 lbs, resulting in localized pressure points and potential tissue damage.
- Pressure Redistribution Effectiveness
The pressure redistribution capabilities of the bedding are calibrated based on the specified weight capacity. Exceeding this limit disrupts the intended pressure distribution pattern, concentrating pressure on certain areas and negating the benefits of the specialized design. This is particularly problematic for patients with limited mobility or sensory deficits, who may be unable to perceive or communicate discomfort. An air-fluidized surface designed to evenly distribute weight across the entire surface area will not function as intended if the patient’s weight exceeds the recommended limit, leading to uneven pressure distribution and increased risk of skin breakdown.
- Bed Frame Compatibility and Stability
The weight capacity of the bedding must be considered in conjunction with the weight capacity of the swing bed frame itself. Overloading the bed frame can compromise its stability and functionality, potentially leading to mechanical failures, such as broken support structures or malfunctioning adjustable features. This creates a hazardous environment for both patients and caregivers. For example, if a bed frame is rated for a maximum load of 400 lbs (including the weight of the bedding and the patient), using a specialized surface and accommodating a patient whose combined weight exceeds this limit could lead to structural instability and potential injury.
- Product Longevity and Warranty
Consistently exceeding the stated weight capacity can significantly reduce the lifespan of the specialized bedding and may void the manufacturer’s warranty. Overloading the support surface places undue stress on the internal components, accelerating wear and tear and increasing the likelihood of premature failure. This results in increased replacement costs and potential disruptions in patient care. Routine use exceeding the weight limit may also affect the overall structural stability and the life span of the material.
Adhering to the specified weight capacity is essential for maintaining the integrity and effectiveness of specialized bedding in swing bed units. Failure to do so can compromise patient safety, increase the risk of complications, and lead to unnecessary equipment replacements.
5. Size Compatibility
Size compatibility represents a foundational consideration in the selection and deployment of bedding within swing bed units. A properly sized surface ensures correct fitment on the bed frame, contributing to patient safety, pressure redistribution efficacy, and overall functionality of the adjustable bed. A mismatch in dimensions can lead to several negative consequences. For example, if the bedding is too small, gaps may form between the surface and the bed frame, posing a risk of patient entrapment. Conversely, an oversized surface may overhang the frame, interfering with the bed’s adjustable features and potentially causing damage to both the surface and the frame.
The standard dimensions of hospital beds are typically 36 inches wide and 80 inches long, but variations exist, particularly in bariatric or specialty beds. Prior verification of internal dimension measurements is crucial to avoid mismatch.
Furthermore, size compatibility directly influences pressure redistribution. If the bedding does not fully cover the support structure of the bed frame, localized pressure points may develop, negating the benefits of the specialized materials designed to prevent pressure ulcers. This is especially critical for patients with limited mobility who are unable to reposition themselves independently. Accurate sizing also impacts the effectiveness of bed alarms and other safety features integrated into the bed frame. A surface that is not properly aligned may interfere with the sensors, leading to false alarms or, more critically, failure to detect when a patient is attempting to exit the bed. An example would be the usage of an 84-inch mattress of a bedframe 80 inch, this may compromise the sensors from the bed and affect the pressure redistribution and also the alarms.
In summary, size compatibility is not merely a matter of convenience; it is a fundamental requirement for ensuring patient safety and maximizing the therapeutic benefits of specialized bedding in swing bed settings. Healthcare facilities must establish protocols for verifying surface dimensions prior to deployment and regularly inspect bedding to ensure proper fitment is maintained. Neglecting this critical aspect can lead to preventable complications and increased healthcare costs. Attention to the proper sizing represents a proactive approach to optimizing patient care and minimizing risks in the swing bed environment.
6. Durability
Durability is a paramount consideration in the context of specialized hospital bedding intended for swing bed units. These units, designed for both acute and sub-acute care, subject bedding to frequent use and rigorous cleaning protocols, necessitating a high degree of resilience to maintain functionality and hygiene over extended periods.
- Material Resistance to Degradation
The composition of materials directly influences the longevity of the product. Fabrics and foams must withstand repeated exposure to cleaning agents, bodily fluids, and the physical stresses of patient movement. Inferior materials degrade rapidly, leading to cracking, tearing, and loss of support, compromising both patient comfort and infection control. For example, a surface constructed with high-grade, coated nylon will resist fluid penetration and chemical breakdown far longer than one made with standard vinyl.
- Seam Strength and Construction Integrity
Weak seams represent a common point of failure in hospital bedding. Reinforced seams, utilizing durable stitching techniques and high-tensile-strength threads, are crucial for preventing separation and maintaining the integrity of the enclosure. Compromised seams allow fluid ingress, creating a breeding ground for bacteria and requiring costly repairs or premature replacement. Welding sealing in seams offers a greater level of protection. For instance, mattresses with welded seams can provide superior protection.
- Resistance to Compression and Deformation
The internal components, such as foam cores or air bladders, must maintain their shape and support properties over time, despite repeated compression from patient weight. Materials that exhibit excessive compression set lose their ability to redistribute pressure effectively, increasing the risk of pressure ulcer development. High-density foams with resilient properties are essential for preserving long-term support and pressure redistribution capabilities.
- Impact of Cleaning and Disinfection Protocols
Hospital-grade cleaning agents, while necessary for infection control, can be harsh on certain materials. Surfaces must be able to withstand repeated exposure to these chemicals without degradation of their structural or functional properties. Materials that are easily discolored, cracked, or otherwise damaged by cleaning agents have a shorter lifespan and pose an ongoing infection control risk. For example, some bleach solutions can breakdown standard vinyl or plastic, damaging the mattress. Regular maintenance to ensure maximum life for the mattress is crucial.
The long-term cost-effectiveness and patient safety of specialized bedding are inextricably linked to its durability. While initial purchase price may be a factor, prioritizing materials and construction techniques that ensure resilience and longevity ultimately translates to reduced replacement costs, improved infection control, and enhanced patient outcomes within the swing bed environment.
Frequently Asked Questions
This section addresses common inquiries regarding specialized hospital bedding, specifically concerning its application and performance within swing bed units. The information presented aims to clarify key aspects and provide guidance for informed decision-making.
Question 1: What differentiates a “swing bed mattress” from a standard hospital mattress?
Specialized hospital bedding designed for swing bed units typically incorporates advanced pressure redistribution technologies and durable, infection-resistant materials. These features cater to the needs of patients transitioning between acute and sub-acute levels of care, who often require extended periods in bed. Standard hospital mattresses may lack these specialized characteristics.
Question 2: How does the “swing bed mattress” contribute to pressure ulcer prevention?
Advanced bedding often utilizes materials such as viscoelastic foam, gel-infused layers, or air-filled bladders to conform to the patient’s body and redistribute pressure away from bony prominences. This reduces the risk of localized ischemia and subsequent pressure ulcer formation.
Question 3: What cleaning and disinfection protocols should be followed for swing bed bedding?
Strict adherence to established infection control protocols is essential. Surfaces should be cleaned and disinfected using hospital-grade cleaning agents and techniques recommended by the manufacturer. Regular inspection for tears or damage is crucial to prevent microbial colonization.
Question 4: What factors should be considered when determining the appropriate weight capacity for the bedding?
The stated weight capacity must be adequate to safely support the patient without compromising the structural integrity or pressure redistribution capabilities of the surface. Exceeding the weight limit can lead to premature wear, reduced effectiveness, and potential safety hazards.
Question 5: How does size compatibility impact the performance of the bedding?
Proper dimensions are crucial for ensuring correct fitment on the bed frame. Mismatched sizes can interfere with the bed’s adjustable features, compromise pressure redistribution, and pose a risk of patient entrapment.
Question 6: How often should specialized bedding be inspected and replaced?
Routine inspections should be conducted to identify signs of wear, damage, or deterioration. Replacement frequency depends on factors such as usage intensity, cleaning protocols, and the quality of materials. Manufacturers’ guidelines should be consulted for specific recommendations.
In conclusion, the selection and maintenance of swing bed bedding are critical components of comprehensive pat
ient care. Adhering to established protocols and considering the factors outlined above will contribute to improved patient outcomes and cost-effectiveness.
The following section will explore emerging trends and innovations in specialized hospital bedding technology.
Swing Bed Mattress
This exploration of support surfaces has emphasized their critical role in providing appropriate support, pressure redistribution, and infection control within the unique environment of swing bed units. Key considerations, including material composition, weight capacity, and size compatibility, directly impact patient safety, clinical outcomes, and the operational efficiency of healthcare facilities. Adhering to established maintenance protocols and selecting products based on evidence-based criteria are essential for maximizing the benefits of this specialized equipment.
Given the ongoing advancements in materials science and healthcare technology, continuous evaluation and refinement of bedding selection processes are warranted. Prioritizing patient comfort, safety, and infection prevention through informed procurement and diligent maintenance will contribute to improved quality of care and enhanced resource utilization within the evolving landscape of swing bed programs. Further research and collaboration between clinicians, engineers, and manufacturers are needed to optimize the design and performance of support surfaces, ensuring they meet the ever-changing needs of the patient population.